In his first letter to the Corinthians, St Paul explained, “When I was a child, I spoke and thought and reasoned as a child, but when I grew up, I put away childish things.”[1] Though accepted as an obvious fact of nature, the cause of this transformation in thinking has long provoked deeper questions. Is it due to internal forces in the brain which bring about structural and functional change? Or is it the result of moulding by external experience? Or both?
In current Australian and many other societies, the errant behaviour of children during the process of maturation to adulthood has long provoked practical questions. When should children be held legally accountable for their actions? Should there be an age-based scale of severity of punishments? And, if so, can accountability be generalised to a particular age?
In Australia, in recognition of the “childish brain”, the minimum age of criminal responsibility is held to be ten years[2]. Between the ages of ten and fourteen, on the presumption that a child is incapable of committing a criminal act, he or she can only be convicted if the prosecution can prove the child could distinguish between right and wrong. From fourteen to either seventeen or eighteen years (depending on jurisdiction), adolescents may be held responsible for criminal acts but are subject to a different range of penalties from adults. Other countries have higher ages for accountability.
This essay appears in the latest Quadrant.
Click here to subscribe
In Australia, recognising the trouble an immature brain can inflict on its holder (and others), the legal age for consensual sex is at least sixteen: for driving, sixteen; for joining the army, seventeen; and for drinking alcohol and for gambling, eighteen.
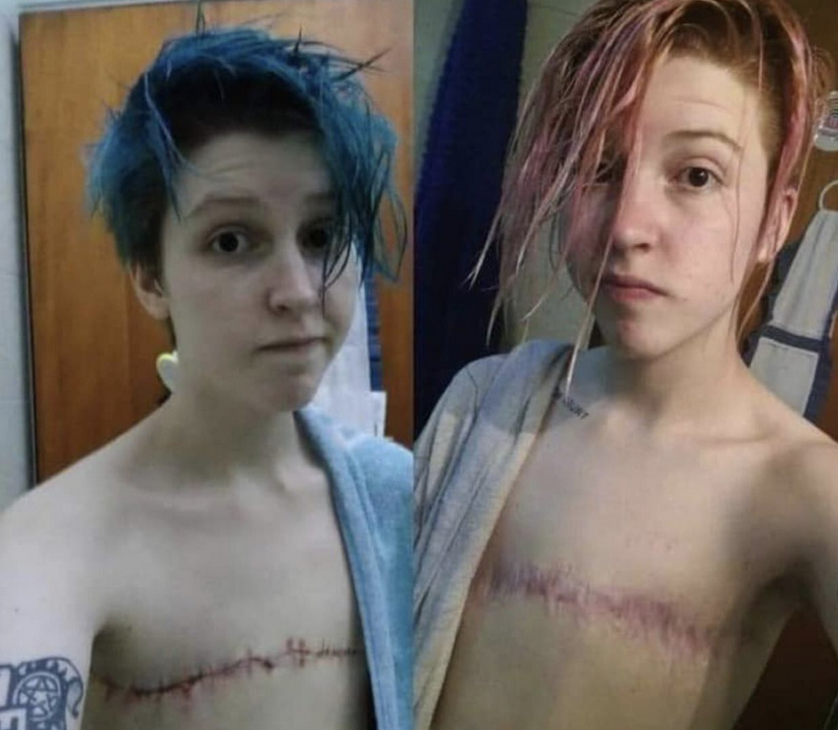
In contrast, in guidelines from the Royal Children’s Hospital in Melbourne[3], there is no age limit for the administration of so-called “affirmation therapy” of a confused child to a gender incongruent with chromosomes. For example, if a child with male chromosomes believes he is a girl, there are no age limits on social affirmation, and on the administration of “puberty blockers”, or of “cross-sex hormones” in pursuit of similitude with the opposite gender. Though mastectomy is generally reserved for those over sixteen, Family Court records reveal that breasts have been removed from fifteen-year-old girls.
A recent report of young people attending the Gender Service of the Sydney Children’s Network, based in Westmead, revealed four had undergone double mastectomy: one, double mastectomy plus hysterectomy; one, breast implantation plus penile skin inversion vaginoplasty; three were considering double mastectomy and two were “booked in with a surgeon” to discuss penile skin inversion vaginoplasty[4].
Gillick competence
As in the UK, credence is given to possession of “Gillick competence”, a term derived from a House of Lords decision regarding the right of a minor to receive contraceptives. Mrs Gillick was protesting against the provision of contraceptives to adolescents under sixteen but the House concluded that a child’s capacity for consent increases with maturity, and parental authority ceases when the child “achieves sufficient understanding and intelligence” for comprehension of what is proposed. This capacity is described as “Gillick competence”, or a “mature minor”.
It is assumption of the validity of “Gillick competence” (or its equivalent) regarding change of gender that underpins the lack of age limits for social affirmation and administration of hormones in the Melbourne guidelines. They are prescribed “in the best interests” of the young person, as judged by parents and staff.[5]
In summary, Gillick competence in gender confusion is the ability of a young person to make an appropriate medical decision. It depends on intelligence, the influence of co-morbid neurodevelopmental, psychiatric and family disorder, the extent of pressures from family, peers and social media, the ability to weigh risk and benefit, and to evaluate longer-term realities, especially sexuality and reproduction.
But is a child’s brain functionally capable of properly making a decision regarding the massive implications of change of gender? Current research on brain development would so “No”.
Scientific advances
Magnetic Resonance Imaging (MRI) provides not only delineation of cerebral morphology but, because of differing magnetic properties between oxygenated and unoxygenated haemoglobin, it can also reveal function. It shows that a child’s brain reaches approximately 90 per cent of adult size by six years, but undergoes extensive remodelling from twelve years to young adulthood[6]. Each lobe undergoes “changes in its composition of grey and white matter, in its connections with other lobes, and in its hormonal environment … according to its own timeline”.
White matter volume in the major lobes increases in a “roughly linear” manner with age, representing the wrapping, by oligodendrocytes, of the axons of neurons in sheaths of myelin, permitting the transmission of messages at speeds up to 100 times those of unmyelinated axons[7].
Grey matter, reflecting neuronal content, is found in two locations: cortical (on the outer surface of the brain) and subcortical (deeper inside). From about six years, cortical grey matter follows an “inverted U” pattern, thickening in accordance with size and complexity of neurons, and then thinning through pruning of neuronal connections for greater rapidity and discretion of function (if at the cost of decreasing capacity for learning).
Changes in subcortical grey matter have been technically harder to quantify. Its basal ganglia and associated limbic systems are integral to emotion, language and memory, and mediate higher cognitive functions, attention and affective states: thus, decision-making. With age, the amygdala increases in size in males, while the hippocampus increases in females, presumably in response to sex hormones secreted from gonads. For example, gonadectomised female rats have a lower density of dendritic spines and decreased fibre outgrowth in the hippocampus, which can be alleviated by hormone replacement[8].
Of relevance to the adolescent brain is the process of pruning of grey matter in the cortex: it occurs first in the primary sensory areas and then progresses anteriorly to involve the prefrontal cortex and superior temporal gyrus. That is, centres “subserving primary functions such as motor or sensory systems mature before the higher-order association areas which integrate them”[9]. Indeed, the dorso-lateral prefrontal cortex does not reach final maturation until the mid-twenties[10], though it is “linked to the ability to inhibit impulses, weigh consequences of decisions, prioritise and strategise”.
Parts of the limbic system are both incompletely myelinated and connected to the decision-making frontal cortex until the mid-twenties. Consequently, the emotional centre is poorly connected to the judgment centre, resulting in the likelihood of decisions being made on emotional grounds, unmodified by reason. Thus “executive function and emotional responses are not just less developed or different in teens: [They] are also less closely linked than in the typical adult brain. As a result, a teen may intellectually understand an issue and emotionally have a response to that issue, but these two processes may occur nearly in parallel rather than in dialogue. Emotional and executive functions must work together to bring about almost any kind of decision”[11].
Many internal and external factors affect brain development, from genetics to nutrition, toxins, drugs and hormones, especially those involved in stress reaction to adverse experiences[12]. Indeed, Adverse Childhood Events (ACEs), including emotional, physical and sexual abuse, neglect and exposure to domestic violence, which disrupt an infant’s “attachment” to primary care-givers, are known to alter the “structure of the developing brain, the expression of genes and subsequent function”[13][14]. Thus, early life experiences may become biologically embedded or internalised into the child’s biology.

It is relevant, at this stage, to consider an earlier publication of the Westmead Gender Service, which concluded that the development pathways of gender-confused children reflected “at-risk patterns of attachment and high rates of unresolved loss and trauma” resulting from ACEs, family disruption and socio-economic disadvantage”[15]. A later publication reported “ongoing mental health concerns” in 88 per cent of its clients[16].
Cold and heat in a “pre-frontal cortex deficit disorder”
Douglas Diekema has emphasised this lack of concordance between cortical and sub-cortical centres: between the “cognitive control system” composed of pre-frontal and parietal cortical structures and the “socio-emotional system” composed of limbic and para-limbic structures. He says the former tends to be “consciously controlled, volitional, deliberate, reasoned, analytic and reflective” requiring more “time and conscious effort” than the “socio-emotional” system which tends to “involve rapid, automatic processing that is often reactive, intuitive and unconscious, picking up patterns before an individual may be consciously aware of them, and motivating behaviour change through feelings and autonomic responses”[17].
Noting that the systems mature “along different trajectories” (with socio-emotional maturing with puberty and cognitive control during the mid-twenties) Diekema declares that “adolescents experience what may be called a “pre-frontal cortex deficit disorder” in which: the ability to regulate and understand emotions remains underdeveloped; susceptibility to peer pressure influence is greater; the ability to delay rewards is limited; and adolescents and young adults are more likely than adults to engage in a variety of risky behaviour (such as binge drinking, smoking, casual sex, violent or criminal behaviour and dangerous driving).
The cognitive control system has been likened to a “cold” process, compared to the “hot” socio-emotional process. Diekema implies that cognitive decisions made in a “cold” environment by a fourteen-year-old may not be the same as those made in the “heat” of emotionally charged situations or under pressure exerted by peers, family members or spiritual community members, when “adolescent decision-making is often less than optimal” (and may be more of a reflection of the desires of others, rather than those of the adolescent).
Regarding medical decisions, Diekema declares, “As a general rule adolescents may require limits on the kinds of decisions they are allowed to make.” He concludes:
The current age of majority (18 to 21 years of age depending on the state [in the US]) is not clearly supported by empirical data, at least for some decisions. It may well be that [it] should be reconsidered … the data establish fairly clearly that most adolescents younger than the legal age of majority have not yet attained a level of brain maturation that justifies treating them like adults with respect to significant, potentially life-altering health care decisions.
Other physiological influences on decision-making
As well as changes in neurons and myelination during adolescence, there are changes in hormones and neurotransmitters that affect both emotion and executive function. Both testosterone and oestrogen have receptors in the brain, organising and activating patterns set down before birth.
In a cascade of hormonal interaction, the sex hormones are released from the gonads in response to hormones released from the pituitary gland, whose release is stimulated by Gonadotrophin Releasing Hormone (GnRH) from the hypothalamus, whose release is stimulated by a neuropeptide, kisspeptin, in response to other factors. All these hormones, and the neurotransmitter, kisspeptin, are involved in gender identity and sexualisation through effects on the brain.
Furthermore, the neurotransmitter dopamine, which is most responsible for feelings of pleasure, is affected by brain changes in adolescence. During maturation its levels in the pre-frontal cortex are not matched by those in the limbic reward centre, “suggesting the adolescent requires more excitement and stimulation to achieve the same level of pleasure as an adult” thus provoking risky behaviour and unwise decisions.[18] Secretion of dopamine is basic to addiction, hence the proclivity to its various forms in adolescence.
Transgendering: a life-altering decision
An egregious example of a “significant, potentially life-altering health care decision” mentioned by Diekema is surely that of social, hormonal and surgical “affirmation” of an adolescent to a gender incongruent with chromosomes. Not only is lack of concordance between major parts of the brain likely to impair judgment, other factors are also influential.
The first is the presence of co-morbid neurodevelopmental disorders which have long been known for association with gender dysphoria[19][20][21][22][23][24]. These include autism, depression, anxiety and even frank psychosis. As mentioned above, disruption of early infantile attachment to a primary carer is prevalent in children with gender dysphoria[25] and associated with lasting neurobiological effects. Summarising, Newman et al[26] report disruption in metabolism in regions involved in stress regulation including the orbito-frontal cortex and its innervation and connectivity with the limbic system. That is, between the centres of cognitive control and emotional drive. And then there is the impact on growing brains of alcohol, marijuana[27] and other drugs, all of which may affect the precarious balance of emotion and cognitive control in the immature brain.
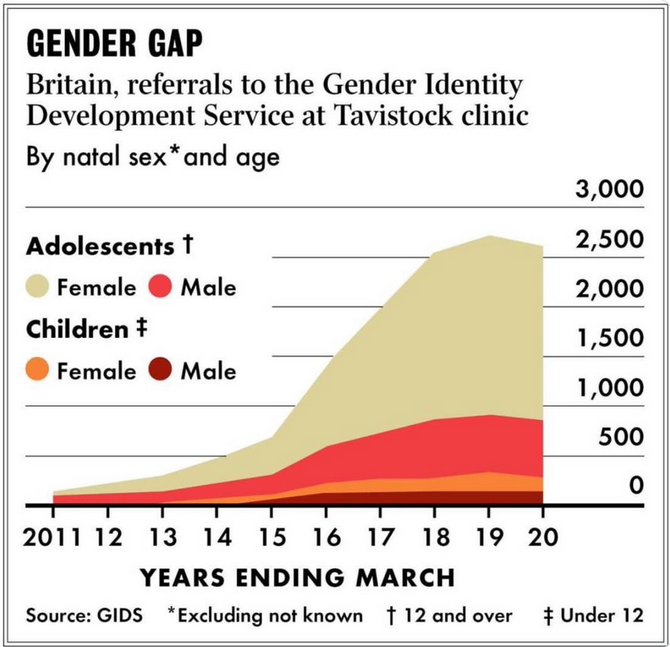
The second factor is the lack of information upon which to make an informed decision. One un-emphasised problem with the Gender Identity Service based in the Tavistock Clinic in London is its sustained failure to publicise the proven side-effects of blockers and cross-sex hormones. I am personally aware of this “silence”, having had access to its “information” packages in preparation for a court submission on behalf of the transgendered Keira Bell.
The silence is, however, not confined to Tavistock. The mantra that “blockers are safe and reversible”, with failure to mention cerebral effects of both blockers and cross-sex hormones, characterises publications from the Children’s Hospital in Melbourne, and the recent LGBTIQ+ “Health Strategy” of the New South Wales government.[28][29]
Even the commendably cautious “Follow-up Study” from the Gender Service at Westmead, while reporting a negative effect of blockers on bone density, merely declares “far less is known … about effects on cognitive, psychosocial and psychosexual development and mental health functioning”[30]. Has no one in those prestigious institutions searched the literature for such effects, as will be discussed below?
A third factor is “peer pressure”. The current epidemic of childhood gender dysphoria is fairly described as a “social contagion”,[31] spread in social media and friendship groups. Furthermore, it is observed that, once the initial phase of social affirmation to gender incongruent with chromosomes has been entered, most children progress to puberty blockers and then cross-sex hormones. In this progression, “peer pressure” appears insurmountable. It comes from friends and colleagues but may emanate from parents, teachers, social and ordinary media, legislation, and gender clinic staff, all applauding and supporting the change in gender of a vulnerable child, dissuading a change of mind.
Now that “Christian faith” schools are pressured to participate in social affirmation[32], “divine approval” may appear to augment “poster child” popularity, confirmed by the granting of new names and pronouns, cross-uniforming, special toilets, and entry into the sporting ranks of the opposite chromosomes. Psychologically, how can the child change its mind?
The fourth factor is the physical effect of blocking GnRH. In peri-pubertal sheep, it causes hypertrophy of the limbic system, associated with disruption in many genes, expressed behaviourally in increased emotional lability, interruption of memory, and fearful preference for the familiar, rather than the novel[33][34][35][36][37]. Other studies report disruption of neuronal function in laboratory specimens[38], on the structural development of the brain[39], on the integrity of neurons in extra-cranial sites[40], on the development of sexuality [41] and even on cerebral ageing and associated dementia[42][43][44]. There is now a trial on the giving of GnRh to children with Down syndrome, on the basis of rodent models suggesting its lack is associated with dementia.
Regarding transgendering children, the “familiar”, of course, is prior social affirmation. which is preferred to the “novel” concept of re-orientation with chromosomes. Thus, animal studies add physiological to psychological explanation for the observed likelihood of progression up the stages of hormonal transgendering. Westmead reports occurrence in 77.6 per cent of clients.
Westmead’s researchers wonder if such progression reflects accuracy of diagnostic screening rather than the “dynamic of a self-fulfilling prophecy”, concluding that “outcome data many years down the track are needed to clarify this complex question”. They admit that “the evidence base for all aspects of treatment was sparse, especially relating to long-term outcomes” and declare their own study was limited because it was only “a naturalistic follow up study … without … a control group … and did not use a blinded, randomised approach”. Appropriately, the authors declare that “the consequences of receiving gender-affirming medical interventions … are likely to be life changing”, admitting that, if the choice for affirmation “was not the right one … it may seriously distort both the young person’s life choices and on-going sense of well-being”.
The question must then be asked of all gender services in children’s hospitals: is the magnitude of intervention based on the “minitude” of supporting evidence, in the face of reported cerebral side-effects, under the say-so of an already pressured immature brain, complicated by mental disorder, something that should be continued “for years” in search of justification through unregulated studies?
A fifth factor interfering with decision-making can be inferred from the observed effects of cross-sex hormones on adult brains: male brains have shrunk at a rate ten times faster than ageing, after only four months administration of oestrogen.[45] The female brain hypertrophies on testosterone. Such structural alteration may be expected to affect function. That the rate of suicide by transgendered adults is reported to be some twenty times that of the general population[46][47] is claimed, by proponents, to represent societal ostracism. It could, however, represent failure of an iatrogenically altered brain to find “gold” at the foot of the rainbow.
That such shrinkage should fail to be mentioned in literature or media supporting transgendering is a matter of wonder. What fuss might have erupted if Covid vaccines had been found to shrink the brain, even a little bit, without acknowledgment?
Conclusion
The lack of concordance between socio-emotional and cognitive centres of control has been described as a “maturity gap” in which adolescents have made regrettable decisions. Historically, society has tried to minimise the proclivity to harm by legislative and other means but, now, what might be called a “utopian ideology” of unrestricted sexuality, including transgendering, has been permitted, indeed encouraged, by activists within government and its institutions, to be promoted with evangelical zeal to children and adolescents whose brains are known to be influenced more by feelings than facts.
To its credit, the Gender Service of the Sydney Children’s Network is propounding a “neutral therapeutic stance that communicates the possibility of multiple developmental pathways and choices”. And it “highlights the importance of comprehensive screening and the value of a comprehensive biopsychosocial (including family) assessment … that is crucial in exploring the many different factors—predisposing, precipitating and maintaining … that have contributed to the young person’s distress”. It emphasises the need for “ongoing supportive psychotherapy which [acts] as a ‘safety net’ … helping young persons to navigate their own development”. This appears to mean psychotherapy might render the child comfortable with a gender assigned by chromosomes: that the child might change its mind and not pursue “affirmation”.
The Westmead report refers to the “individualised psychosocial interventions (e.g. psychoeducation, individual therapy, school-home liaison, family therapy)” offered by the National Association of Practising Psychiatrists which urges that “first line treatments” should be undertaken before experimental puberty-blocking drugs and other medical interventions are considered. Thus, psychotherapy and help with co-morbid mental problems might produce feelings congruent with chromosomes.
Starkly opposite, the gender clinic in Melbourne supports the “gender affirmative model” in which “decision making should be driven by the child”. And this “progressive” concept is apparently shared by the New South Wales Ministry of Health.[48] The Melbourne model is substantiated by Victorian legislation (supported by both major political parties) that forbids alternatives to affirmation, and intimidates anyone who thinks differently. It declares that no sexual preoccupation represents a weakness or a defect (or certainly a sin) that needs fixing. And it promises up to ten years incarceration and great fines for anyone attempting to “change or suppress” such preoccupation in another.[49]
Thus, it is a criminal act to provide psychotherapy, or any counselling, or any spiritual help, by anyone (including parents) to anyone distressed by unwanted sexual or gender preoccupations, even if help is requested, informed and voluntary. Moreover, the crime of helping someone suppress unwanted desires or of helping a confused child become comfortable with the reality of its chromosomes, is alleged to be so destructive it warrants reversal of the democratic tradition of “onus of proof” from being innocent until proven guilty, to being guilty until proven innocent. Clearly, the Westmead unit should avoid southward translocation.
Victoria has legislated in favour of the “hot part” of the brain, criminalising efforts to develop “the cold”. To refer to the ideas of Viktor Frankl, the Jewish psychiatrist who survived Auschwitz to propound his theory on the need for a “meaning” for living: man should have the freedom to “decide for himself” and be educated to make appropriate decisions, and acknowledgment of the reality of instincts must presuppose freedom to reject them[50]. To refer to Sigmund Freud, Victoria promotes the “id” and criminalises the “superego”.
Regrettably, from an early age, Australian children are exposed to skilled presentations that declare they may not be the boy or girl they were “assigned” at birth: that sexuality should not be confined to a Judeo-Christian worldview (or, for that matter, an Islamic one). And parents, counsellors, therapists and pastors are warned (intimidated) that attempts to “change or suppress” whatever sexual orientations might emerge from such propaganda constitute a serious criminal offence.
This message of gender and sexuality is amplified in the media, between advertisements for alcohol and gambling, and marijuana is declared “medicinal” by doctors’ organisations. The onslaught during the “maturity gap” has, indeed, many fronts!
Instead of these societal messages bringing liberation, the tragic reality is that Western young people are becoming afflicted by mental disorder at an alarming and unprecedented rate. [51] The challenge for Christians is the delivery of the Good News, with its promise of both forgiveness and new life, assured in other words of St Paul, that if “anyone is in Christ, he is a new creature; the old things have passed away; behold, new things have come”. [52] Some old things have, however, not passed away: the need for courage to deliver such messages, contrary, as they are, to the power of utopian states. And the obligation to care for children in distress.
This is an edited version of an address to the International Christian Medical Association in February. Dr John Whitehall is a professor of paediatrics at a university in Sydney. He has written several articles for Quadrant on childhood gender dysphoria.
[1]1 Corinthians 13:11.
[2] Urbas G, The age of responsibility. https://www.aic.gov.au/sites/default/files/2020-05/tandi181.pdf. Accessed February, 2023.
[3] Telfer MM, Tolit MA, Pace CC, Pang KC. Australian Standards of Care and Treatment Guidelines for Trans and Gender Diverse Children and Adolescents. Version 1.3 Melbourne.: The Royal Children’s Hospital, 2020.
[4] Elkadi J, Chudleigh C, Maguire AM et al. Developmental choices of young people presenting to a gender service with gender distress: a prospective follow-up study. Children. 2023. 10, 314. https://doi.org/10.3390/children10020314.
[5] https://www.rch.org.au/uploadedFiles/Main/Content/adolescent-medicine/australian-standards-of-care-and-treatment-guidelines-for-trans-and-gender-diverse-children-and-adolescents.pdf
Gillick v West Norfolk and Wisbech Area Health Authority and Department of Health and Social Security: HL 17 Oct 1985.
[6] Blakemore S-J. Imaging brain development. The adolescent brain. NeuroImage. 2011. Doi:10.1016/jneuroimage.2011.11.080 in The teenage brain under construction. American College of Pediatricians. https://acpeds.org/position-statements/the-teenage-brain-under-construction. Accessed23/6/2022.
[7] Giedd JN. Structural magnetic resonance imaging of the adolescent brain. Ann NT Acad Sc. 2006; 1021 (1):77-85
[8] Gould E et al. Gonadal steroids regulate dendritic spine density in hippocampal cells in adult. J Neurosc. 1990. 10:1286-1291.
[9] Giedd op cit.
[10] National Institute of Mental Health. Teenage brain: a work in progress. NIH http://www.nih.gov.gov/health/publications/teenage-brain-a-work-in-progress-fact-sheet/index.shtml.
[11] Pustilnik AC, Henry LM. Adolescent medical decision making and the law of the horse. J Health Care Law and Policy. 2012;15:1-14./
[12] Giedd. Op Cit.
[13] Shonkoff JP. Capitalizing on advances in science to reduce health consequences of early childhood adversity. JAMA 2016.170(10):1003-1007.
[14] Seso-Simic et al. Recent advances in the neurobiology of attachment behaviour. Translational Neuroscience. 2010.1 (2):148-159. DOI:10.2478/v10134-010-0020-0.
[15] Kozlowska K, Chudleigh C, McGuire G et al. Attachment patterns in children and adolescents with gender dysphoria. Front. Psychol. 2021. 11:582688. Doi:10.3389/fpsyg.2020.582688.
[16] Kozlowska K, Chudleigh C, McGuire G et al. Developmental pathway choices of young people presenting to a gender service with gender distress: a prospective follow-up study. Children 2023,10,314. https://doi.org/10.3390/children10020314.
[17] Diekema D. Adolescent brain development and medical decision making. Pediatrics 2020. 146 (s1):s 19-24.
[18] American College of Pediatricians. Op cit.
[19] Wallien MS, Swaab H, Cohen-Kettenisk PT. Psychiatric co-morbidity among children with gender identity disorder. J Am Acad Child Adolesc Psych. 2007;46(10):1307-1314.S
[20] Becerra-Culqui T, Liu Y, Nash R et al. Mental Health of Transgender and Gender Nonconforming Youth Compared With Their Peers. Pediatrics 2018. 141(5). DOI:10.1542/peds.2017-3845.
[21] Kaltiala R, Sumia M, Tyolajarvi M et al. Two years of gender identity service for minors: overrepresentation of natal girls with severe problems in adolescent development. Child Adol Psych Mental Health. 2015.9(9). Doi 10 1186/s13034-015-0042-y.
[22] De Vries AL, Noens IL, Cohen-Kettenis et al. Autism spectrum disorders in gender dysphoric children and adolescents. J Autism Dev Dis. 2010;40:930-936.
[23] Holt V, Skagerberg E, Dunsford M. Young people with features of gender dyshoria: demographics and associated difficulties. Clin Child Psychol Psychiatry. 2016;164:108-118.
[24] Chen M, Fuqua J, Eugster E. Characteristics of referrals for gender dysphoria over a 13-year period. J Adolesc Health. 2016;58(3):369-371.
[25] Kozlowska K, Chudleigh C, McClure G, Maguire AM and Ambler GR (2021) Attachment Patterns in Children and Adolescents With Gender Dysphoria. Front. Psychol. 11:582688. doi: 10.3389/fpsyg.2020.582688
[26] Louise Newman, Carmel Sivaratnam & Angela Komiti (2015) Attachment and early brain development – neuroprotective interventions in infant–caregiver therapy, Translational Developmental Psychiatry, 3:1, DOI: 10.3402/tdp.v3.28647
[27] Whitehall J. Medical marijuana: a triumph of hope over experience. Quadrant. July-August. 2022.
[28] NSW Government. NSW LGBTIQ+ Health Strategy 2022-2027. For people of diverse sexualities and genders, and intersex people, to achieve health outcomes that matter to them. Sydney. 2022.
[29] https://www.health.nsw.gov.au/lgbtiq-health/Publications/lgbtiq-health-summary.pdf Accessed March 2, 2023.
[30] Elkaldi J et al. Op cit.
[31] Littman L. Parent reports of adolescents and young adults perceived to show signs of a rapid onset of gender dysphoria. PLoS One, 2018 – journals.plos.org.
[32] Whitehall J. Catholic Bishops Capitulate in Schools Gender Confusion. Quadrant. November 2022.
[33] Nuruddin S, Bruchhage M, Ropstad E et al. Effects of peri-pubertal gonado-tropin releasing hormone agonist on brain development in sheep…a magnetic resonance imaging study. Psychoneuroendocrinology. 2013;38;3115-3127.
[34] Nuruddin S, Krogenaes A, Brynildsrud OB et al. Peri-pubertal gonadotropin-releasing hormone agonist treatment affects sex based gene expression of amygdala in sheep. Psychoneuroendocrinology. 2013;38(12).3115-3127.
[35] Hough D, Bellingham M, Haraldsen I et al., 2017 Spatial memory is impaired by peripubertal GnRH agonist treatment and testosterone replacement in sheep. Psychoneuroendocrinology. 2017; 75:173-182.
[36] Wojniusz S, Vogele C, Ropstad E et al. Prepubertal gonado-tropin-releasing hormone analog leads to exaggerated behavioural and emotional sex differences in sheep. Hormones and Behaviour. 2011;59:22-27.
[37] Anacker C et al. Behavioural and neurobiological effects of GNRH agonist treatment in mice-potential implications for puberty suppression in transgender individuals. Neuropsychopharmacology. 2021;46:882-890.
[38] Prange-Kiel J, Jarry H, Schoen M et al. Gonadotrophin releasing hormone regulates spine density via its regulatory role in hippocampal oestrogen synthesis. J Cell Biol. 2008;180:417-426.
[39] Schneider MA et al. Brain Maturation, Cognition and Voice Pattern in a Gender Dysphoria Case under Pubertal Suppression. https://doi.org/10.3389/fnhum.2017.00528. Front Hum Neurosci. 2017.11
[40] Ohlsson B. GonadotropinReleasing Hormone and Its Role in the Enteric Nervous System. Front. Front Endocrinol (2017) June 7; 8: 110.
[41] Whitehall J. Reviewed in Catholic Bishops Capitulate in Schools Gender Confusion. Quadrant. November 2022.
[42] Zhang G, Li J, Purkayastha S et al. Hypothalamic programming of systemic ageing involving IKK-b, NF-kB and GnRH. Natiure, 2013;497:211-216.
[43] Zhang G, Li J, Purkayastha S et al. Hypothalamic programming of systemic ageing involving IKK-b, NF-kB and GnRH. Natiure, 2013;497:211-216.
[44] Manfredi_Lozano M, Leysen V, Adamo M et al. GnRh rescues cognition in Down Syndrome. Science. 2022;377:eabq4515
[45] Hulshoff Pol HE, Cohen-Kettenis PT, Van Haren NE, et al. Changing your sex changes your brain: Influences of testosterone and estrogen on adult human brain structure. Eur J Endocrinol. 2006;155(1):S107–S111. Doi 10.1530/eje.1.02248
[46] Dhejene C, Lichtenstein P, Boman M et al. Long-Term Follow-Up of Transsexual Persons Undergoing Sex Reassignment Surgery: Cohort Study in Sweden. PLOS 1. 2011;6(2):e16885. Doi 10.1371/journal.pone.0016885
[47] De Cuypere, Elaut E, Heylens G, et al. Long term follow up: psychosexual outcome of Belgian transsexuals after sex reassignment surgery. Sexologies. 2006;15:126-133.
[48] NSW Op cit.
[49] Victorian Change or Suppression (Conversion) Practices Prohibition Act 2021 https://content.legislation.vic.gov.au/sites/default/files/2021-02/21-003aa%20authorised.pdf
[50] Frankl V. The doctor and the soul. From psychotherapy to logotherapy. Souvenir Press. 1969. Reprinted 2021.
[51] The Lancet. Protecting the mental health of youth. 2022;12:100306. https://doi.org/10.1016/j.lanepe.2021.100306
[52] 2 Corinthians 5:17.
 Sign In
Sign In 0 Items (
0 Items ( Search
Search










I had to wander off to my local library to find the two word’s I thought I was looking for- where did I find them?
In a dictionary of course!
What should those word’s be?
I wrapped my arms around the heart and the word surfaced seamlessly in the mind.
Dr John Whitehall expressed both, honesty and excellence.
Inner word -brilliant.
Where there is life there is hope. Epoch Times reports: “Idaho’s governor signed a bill on Tuesday criminalizing gender-affirming medical care for transgender minors”. Under a similar Tennessee law, doctors are prohibited from providing gender-affirming care to anyone under the age of 18, including prescribing puberty blockers and hormones. Needles to say, the American Medical Association and the American Academies of Pediatrics and Psychiatry have predicted disastrous consequences from laws such as these, including a pandemic of suicides among transgender teens.
If psychology could safely empty the prisons, we could take it seriously. Instead, now, Prof. Whitehall seems to feel a need to talk in terms of brain anatomy. Of course, material processes in the brain correspond with psychical processes, but the character of the correspondence is largely unknown because the character of the psychical processes is scarcely understood. The perfect playground for the Marxist plan to punish and destroy society.
The destruction of our children’s well-being is the direct consequence of parents abandoning their duty and handing over their children to toxic institutional vehicles, such as schools, television and social media, to guide and influence.
History will show that the suicide of western civilisation began with the embrace of identity politics, beginning with feminism and proceeding through homosexuality to self selected gender.
I wonder whether we will be able to self select our race, as Professor Bruce Pasoce has done, when the Voice is upon us.